At the September meeting of the European Association for Cardio-Thoracic Surgery Meeting three year follow-up data of the SYNTAX trial [9] were presented. I have commented repeatedly on both SYNTAX and reactions it provoked in the professional literature and the lay press [4], [5], [6],[7],[8].
In this analysis, the SYNTAX score was used to separate patients into three groups. This is a risk stratification score based entirely on coronary anatomy and lesion characteristics largely irrelevant for CABG, thus essentially creating non comparable groups for surgery. Despite this, only the lowest scoring group had equivalent outcomes, with the intermediate and high risk groups clearly showing a survival benefit if CABG was performed:
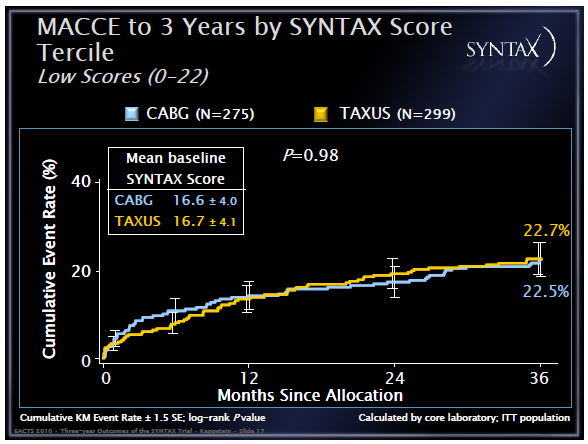
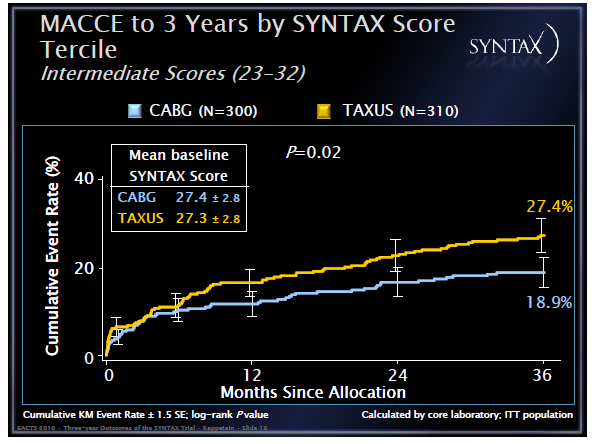
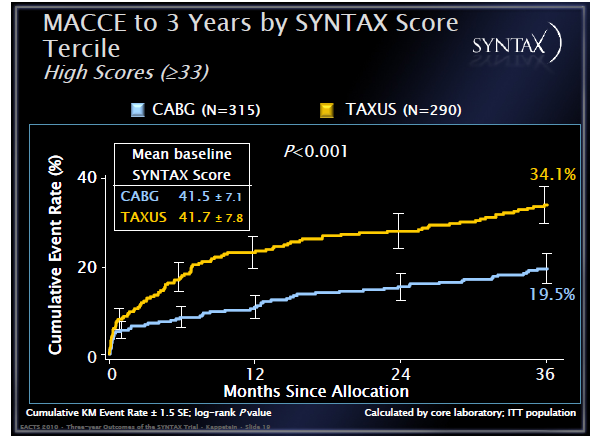
Not surprisingly, for the benefit of cardiologists, the fact that in lowest risk patients PCI seems to perform equally well as CABG was emphasized, while surgeons were enticed by superior outcomes in most other risk factors.
Cardiologists, in control of the board, are not too worried that future results will influence what procedure will be used. Dr. Boden, lead author of the controversial COURAGE trial and trying to establish the benefits of Optimal Medical Therapy for Chronic Stable Angina, during a Wall Street Journal Interview early this year: “What’s going to continue to drive practice is reimbursement.” [1]
Surgeons, who usually are very careful to not offend those who refer them patients, have spoken out this time on the SYNTAX results:
“Despite these findings, it is apparent that their translation (i.e. the choice of PCI vs. CABG) into practice is being heavily influenced by various stakeholders whose belief systems are unfulfilled by the evidence... There are consistent and abundant data to establish that CABG is the standard of care for 3-vessel disease or left main disease, or both.” [2]
“Dr. John Conte, associate director of cardiac surgery at Johns Hopkins Hospital in Baltimore, noted that it is now incumbent on physicians to make sure patients have all the facts before they undergo any procedure. “It’s absolutely amazing that the federal government and private insurers don’t insist on it,” he said. “Wouldn’t it make sense to do the right procedure the first time, rather than do it over and over and drive up the cost of healthcare? To me, it’s a no-brainer.”[3]
As SYNTAX has two more years to go, I expect that differences, already present in year one, will continue and become more obvious in the coming years. Comments in defense of PCI have already included that “outdated” stents were used, therefore the results meaningless. Similar statements will undoubtedly be repeated in the years to come. In this respect it is interesting that in this type of literature, evolving technology only seems to involve PCI, not CABG, as if the procedure in 2010 has not changed since it was introduced in the seventies!
Peri-operative management, especially of ever sicker patients, On-Pump, Off-Pump, Minimally Invasive procedures, the use of arterial grafts, and especially the Internal Mammary Artery grafts have all contributed to what is still – even in the Cardiology literature – referred to as the Gold standard of coronary interventions, so why has this not translated into surgery for those who need it? The answer of this neglect is of course because, at 1.3 million PCI procedures/year, the stent industry (with expected revenues at an expected $15B/year) heavily sponsors the use of PCI and not CABG.
If there is a trend in the recent stent literature, it is that unwanted outcomes of a trial invariably result in requests for more data, complaints of poor patient selection and/or analysis and especially, the request for more studies.
Like in politics, one way to make sure nothing will happen is to create a committee (or write more papers) to study the problem!
Please let me know what you think,
Dr T
Rererences:
[1] A Simple Health-Care Fix Fizzles Out. Keith Winstein, February 11, 2010, The Wall Street Journal
[2] Treatment Selection for Coronary Artery Disease: The Collision of a Belief System with Evidence, Peter K. Smith, Ann Thorac Surg 2009;87:1328–31
[4] Copy of a letter to the Editor, Wall Street Journal 2/22/2010
[5] Stents Downgraded by Wall Street Journal: If Only It Were That Simple
[6] Point-Counter point, July 14, 2010
[7] Three-year SYNTAX results extend CABG’s superiority over PCI
[8] The SYNTAX Trial

