- Introduction & Anatomy
- Symptoms
- Causes
- Medical conditions
- Controllable causes
- Uncontrollable vauses
- Treatment
- Prevention
- Carotid endarterectomy
- Medications
- ACLS stroke information and Treatment Algorithms
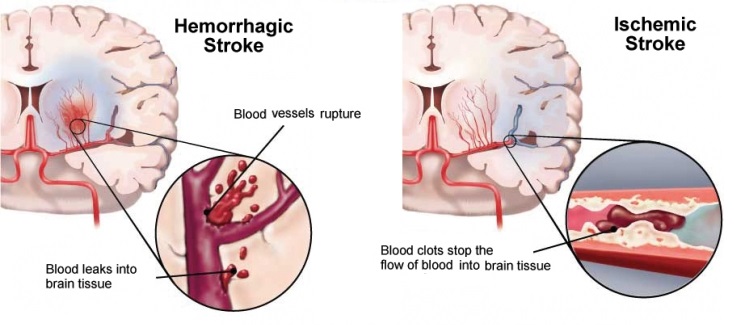
A Stroke occurs when blood flow to a part of your brain is disrupted. A stroke is usually defined as two types:
- Ischemic (caused by a blockage in an artery)
- Hemorrhagic (caused by a tear in the artery’s wall that produces bleeding into or around the brain)
The brain needs a constant supply of oxygen and nutrients in order to function. Even a brief interruption in blood supply can cause problems. Brain cells begin to die after just a few minutes without blood or oxygen.
Common stroke symptoms seen in both men and women:
- Sudden numbness or weakness of face, arm or leg — especially on one side of the body
- Sudden confusion, trouble speaking or understanding
- Sudden trouble seeing in one or both eyes
- Sudden trouble walking, dizziness, loss of balance or coordination
- Sudden severe headache with no known cause
The major treatable risk factors for cerebrovascular atherosclerotic disease and stroke (CVA) are similar to those for CAD.
Medical conditions that increase your stroke risk:
- Previous stroke or “mini-stroke” (transient ischemic attack, TIA).
Depending on the most likely cause of your stroke, your doctor may prescribe specific medication or consider surgery to remove fatty deposits in your carotid artery. - High blood pressure.
Hypertension is one of the leading risks for heart disease and stroke. Your physician may advise dietary or lifestyle changes, or specific medications to lower your blood pressure. - Diabetes.
High blood sugar can increase your risk, so you should work closely with your doctor to manage it. Learn more about diabetes from the - Heart disease.
If you have an irregular heartbeat (atrial fibrillation), disease of the heart valves, congestive heart failure or have had a recent heart attack, your physician may prescribe medications to thin your blood and/or reduce your cholesterol level.
- Diet
- Smoking
- Hypertension
- A high cholesterol
- Diabetes
- Obesity
- Physical inactivity
- Alcohol use
- Weight loss
- Exercise
The risk is particularly increased in patients with two or more of these risk factors.Control of risk factors for CAD also reduces the risk of stroke.
The mainstay of stroke prevention is management of the potential risk factors:
- Smoking cessation,
- Treatment of high blood pressure,
- Heart disease,
- Control of Diabetes.
A carotid endarterectomy is a surgical procedure in which a doctor removes a stenosis (blockage) from one of the two carotid arteries in the neck. These blood vessels supply blood to a major part of the brain.
Carotid endarterectomies are performed to prevent stroke. Theoperation is particularly beneficial for persons who have already had a stroke or experienced the warning signs of a stroke and have a severe stenosis of 70 percent to 99 percent. In this group, the estimated 2-year risk of stroke is reduced by more than 80 percent.
In most cases, the a carotid stenosis can be detected during a normal checkup. Some of the tests include doppler ultrasound (ECHO) and Arteriography.
Antiplatelets: Platelets are blood cells that help the blood to clot and prevent or stop bleeding in case of an injury. These platelet cells need chemicals produced by the body such as vitamin K and other clotting factors to make them stick together. In a patient who has had a stroke or is at risk (TIA) blood thinners are used to decrease the possibility of the body forming another clot in the blood that may lead to another stroke. Specific antiplatelet drugs used for stroke prevention:
- Aspirin (acetylsalicylic acid, ASA)
- Clopidogrel Plavix®)
- Dipyridamole (Aggrenox®, Persantine® and others)
- Ticlopidine (Ticlid®)
Thrombolytics: Patients who present to the hospital within 3 hours of the first sign of a stroke may be able to receive Tissue plasminogen activator (tPa), a clot-buster that can restore blood flow to the area of the stroke. It can reduce the severity of ischemic stroke if it is given within three hours of stroke onset.
Anticoagulants: A class of drugs used to prevent the blood from forming dangerous clots that could result in a stroke. Often called “blood thinners,” anticoagulants are often the first medication prescribed by doctors following a stroke.
Specific Anticoagulant drugs:
Heparin: can be given intravenously or sub-cutaneously, but not by mouth. Heparin is sometimes used to reduce acute stroke damage or stroke risk in hospitalized patients. In addition, heparin may be used in hospitalized stroke patients to reduce the risk of blood clots forming in leg veins.
Warfarin (Coumadin) is taken by mouth. Daily use of warfarin can reduce the risk of stroke in certain patients, such as patients with atrial fibrillation.
For further reading please consider the the following pages, provided by the ACLS Training Center: