In a new study, Small Coronary Vessel PCI outcomes, the authors identified coronary arteries < 3mm in diameter as an independent risk factor for early restenosis. Quoting an article published in 1996:“small arteries remains a major challenge to revascularization procedures, as coronary artery bypass grafting(CABG) is limited by high rates of technical failure”, they then identified DES as superior to BMI stents in this situation.
While I have no argument with the latter, I have a major issue with the first statement, not because size doesn’t matter (it does even here), but because it compared <3mm PCI procedures with <1.5 mm CABG.
I know this study well because I was part of the study group that published its results.
Here are the outcomes as published by the NNECDSG, a voluntary research consortium representing five medical centers in Maine, New Hampshire, and Vermont of 1325 consecutive patients from one center who underwent CABG between July 1987 and April 1989. I was a co-founder of this organization:
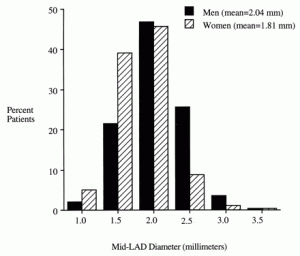
Out of 1325 patients, only 43 (3%) qualified for the criteria in the PCI study, with mid LAD diameters for men 2.04 mm and women 1.81 mm.
While perfectly true that Mid-LAD diameter was inversely related to in-hospital mortality, with the mortality substantially higher in the smallest vessel-size category (1.0 mm: 15.8%) compared with those in the middle (1.5 to 2.0 mm: 4.6%) and largest (2.5 to 3.5 mm: 1.5%) categories (P[trend]<.001), it is difficult compare these results with the restenosis rate of PCI performed in arteries 300% larger!
This NNECDSG study only examined mortality, not graft failure rates or other risk factors. However, many others have shown a 10-15 year graft patency rate of 95% or4 better for Internal Mammary artery grafts and 75-90% for vein grafts, a much more impressive result than PCI failures of 10%/year.
The unwary reader could also easily conclude that CABG performance would be equal to PCI in this size range, while in reality this situation is exceedingly rare. Particularly, Obtuse marginal branches of the circumflex, or RCA frequently were not only hard to reach, but more likely to be in the 1-1.5 mm size range. I would have been glad to have a PCI done to those vessels, precisely of course the ones that would be turned down. I am also sure this situation has not changed, and that in fact the incidence of small vessel CABG has only increased, since in real life all the better target vessels are selected for PCI.
The outcome of CABG with good targets (arteries around 1.5-2 mm) depends on primarily heart function as well as a host of other risk factors but is only rarely influenced by graft size if the target vessel is larger than 1.5 mm. Studies such as the one discussed only lead to confusion, and as an excuse to perform high failure rate procedures,
Dr T
http://www.cardiac-risk-assessment.com/
References: