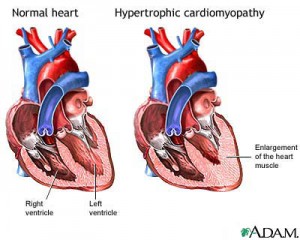
Hypertrophic cardiomyopathy
Question:
My mother-in-law is 64 years old . She has HOCM for the last 3 years with mild to moderate MR and mild LV diastolic dysfunction. She has recently become symptomatic. When she was in the US 3 months back she was admitted in the emergency when she had severe gas, burps, profuse sweating, breathlessness and black-outs. At that point her 2d Echo read Severe MR. She later became all right. She came back to India and her 2D said mild MR. After a month, she had an AICD implantation done. Just prior to that her 2d and MRI said mild to moderate MR. She was doing well,3 weeks later , one fine night she had severe gas, burps n breathlessness for over two hours, cough, couldn’t lie down and was rushed to the hospital. The doctor said it was a diastolic heart failure as she had fluid in the lungs n low blood pressure too. When the 2d was done, it said moderate to severe MR. There was no atrial or ventricular fibrillation. She was in the ICU, but better now. Two days back her 2d echo says mild to moderate MR. Her MR is very fluctuating in the past few months from what we have observed. Doctors are not able to explain the reason for her heart failure and feel that the sudden fluctuation in MR is unusual. Why is that and how can we be sure it may not happen again? The doc says she doesn’t need a surgery now. Please throw some light on this and help us. Your help in this regard will be highly appreciated. Thanks.
Answer:
Your mother-in-law has a complicated problem, and from your description you already know a lot about this disease. Hypertrophic obstructive cardiomyopathy (HOCM) is a disease of the heart muscle that has become thickened (hypertrophied) in places, particularly the septum that divides the left and right side of her heart. In addition, she probably also has an abnormal Mitral valve that may malfunction from time to time.
This is what it looks like:
This condition is associated with a number of potential problems that include:
- Severe rhythm abnormalities, which is why she had a defibrillator implanted to protect against “Sudden Cardiac Death” (SCD).
- Obstruction of the left ventricle during contraction causing diminished blood flow when that happens. Decreased blood flow may cause a range of problems that include tiredness and fainting. In some patients this obstruction may happen at rest, in others only under certain conditions. The latter is known as “dynamic outflow obstruction”, because the degree of obstruction is variable and dependent on the amount of blood in the heart just before contraction. Dynamic outflow obstruction is usually due to an abnormal motion of the Mitral valve called “Systolic Anterior Motion” (SAM).
- Backing up of blood into the lungs when her heart cannot “unload” the blood into the circulation. This will cause Congestive Heart Failure.
- The first symptom of hypertrophic cardiomyopathy among many young patients may be sudden collapse and possible death. Hypertrophic cardiomyopathy is sometimes a cause of death in young athletes who die during heavy exercise.
Tests & diagnosis
Tests may include:
- 24-hour Holter monitor (heart monitor)
- Cardiac catheterization
- Chest x-ray
- ECG
- ECHO
Treatment
Treatment includes medicines such as Beta Blockers, and a defibrillator, if patients appear at risk for SCD. In your mother-in-law’s case, it appears to me that she has a progressive problem with the obstructive part of her disease.
If she continues to fail medical treatment, it may be time to consider either surgery, called Surgical Myectomy, with removal of the obstruction and repair of the Mitral valve, or her doctors may consider an injection of alcohol into the arteries that feed the thickened part of the heart (alcohol septal ablation).
Alcohol septal ablation
Alcohol septal ablation involves injection of alcohol into one or more branches of a coronary artery. This is a technique with results similar to the surgical septal myectomy procedure but is less invasive. In older patients and those with other medical problems, this may be less risky procedure than an operation. This procedures causes a “controlled heart attack”, in which the portion of the septum will contract into a scar.
Cardiac transplantation
In some extreme cases cardiac transplantation is an option.
Her disease is, as you can see, quite complex and will not have a simple solution. It will require an experienced team of physicians, both cardiologists and surgeons to make the right treatment decisions,
Hope this helps,
Dr T
http://www.cardiac-risk-assessment.com/