Introduction
Contents
Heart failure is a decreased ability of the heart to fill and empty. The major purpose of the heart is to circulate blood, which carries oxygen and nutrients around the body, including itself).
Common causes of heart failure include Coronary Artery Disease (CAD), hypertension, heart valve disease and a variety of other causes.
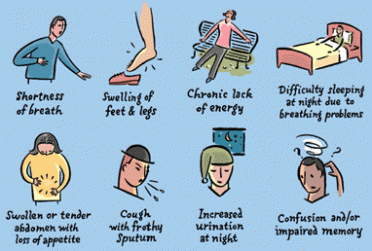
Depending on what part of the heart is involved, impaired pumping may result in fluid retention in your lungs and shortness of breath (Congestive Heart Failure or CHF), or other parts of your body (peripheral edema). When your motor doesn’t work well heart failure is also associated with a decreased ability to do things and early fatigue.
The most common cause of heart failure is CAD.
If heart failure is caused by permanent damage from previous heart attacks, increased blood supply may not help improve heart function. However, if there is impaired blood supply to an otherwise healthy heart muscle, restoring the blood flow back to normal may improve heart function significantly.
Heart failure may be the result of one or many factors. Whatever the cause, it results in the inability to supply sufficient blood flow to meet the body’s needs.

Comments 4
I have a pacemaker installed and I am 70 years old and want to if I can do weights. It’s been three months of my pacemaker installed.
i think in your images you have systolic and diastolic labels reversed. Diastolic typically preserved EF and thick wall whereas systolic is dilated heart with reduced ef.
Author
I am afraid you are wrong!
Dr T
Pingback: Dick Cheney and modern heart failure treatment - Cardiac Health