Question:
Hello, I went to the hospital to the emergency with chest pains. I’m 25, they took tests and returned to tell me I have wolf parkinsons white syndrome. I was wondering how bad this is. I made an appointment with a cardiologist for next week but I can’t stop thinking about it, it worries me.
Answer:
People with Wolff-Parkinson-White (WPW) syndrome are born with an extra connection in the heart, called an accessory pathway, that allows electrical signals to bypass the Atrio Ventricular node and move from the atria to the ventricles faster than usual. The accessory pathway (called Bundle of Kent) may also transmit electrical impulses abnormally from the ventricles back to the atria. This extra connection can disrupt the coordinated movement of electrical signals through the heart, leading to an abnormally fast heartbeat (tachycardia) and other arrhythmias.
Resulting symptoms include dizziness, a sensation of fluttering or pounding in the chest (palpitations), shortness of breath, and fainting (syncope).The most common arrhythmia associated with Wolff-Parkinson-White syndrome is called Paroxysmal Supraventricular Tachycardia (PAT).
Factors that I cannot judge from here determine whether you are at high risk for Sudden Cardiac Death (SCD). Risk factors to look for include previous episodes of unexplained syncope (fainting) or palpitations, and what your EKG looks like during PAT:
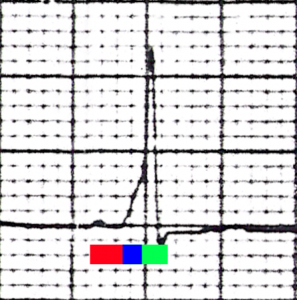
Characteristic EKG finding in WPW Syndrome. The red bar represents the PR interval of 0.1 seconds (100 miliseconds). The blue bar represents the slurred upstroke in the QRS complex that is found in WPW syndrome, known as the delta wave. The combination of the blue bar and the green bar make up the QRS complex, which is prolonged (160 miliseconds).
If indeed you have WPW and since you already have an appointment with a cardiologist, I would assume he or she has decided you are safe during this interval. However, know that not every cardiologist is an specialist in the diagnosis and treatment of WPW, which usually requires an “EP study”, and occasionally a procedure called “radio frequency ablation”.
You might want to also check whether your cardiologist specializes in Electro Physiology, because otherwise you will need to be referred to somebody else and waste extra time,
Hope this helps,
Dr T

Comments 2
After an R.F ablation for W,P,W and SVT some many years ago can the heart REWIRE itself to produce severe atrial irregular rhythms so much so to cause chest pain and light headedness and breathless ness in fact really troublesome and excessive and concerning could it also be that the accessory path way has regrown
Hello Chris, that is possible? 8 years ago I got R.F ablation for both cases WPW and SVT and now I start feeling the way you decribed.
Thanks for clarifying… is that normal?